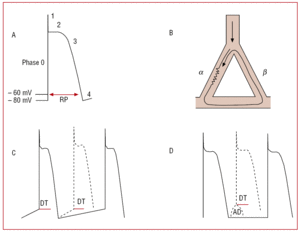
It is rarely used for AF however, its blocking effect on I to has generated interest as a potential therapy for Brugada syndrome and idiopathic ventricular fibrillation. It is a vagolytic and α blocking agent with an intermediate sodium channel blocking effect at rapid heart rates and higher concentrations and a potassium channel blocking effect at slower heart rates and normal concentrations. Quinidine derives from the bark of the cinchona plant and was identified as a potential antiarrhythmic drug a century ago 10 ( Tables 1 and 2). Amiodarone and dronedarone affect a broad range of channels including sodium, calcium, and multiple potassium channels. Sotalol and dofetilide are potassium channel blocking drugs that display reverse use dependence such that repolarization is prolonged at slow heart rates. Propafenone and flecainide have the slowest dissociation kinetics of the sodium channel blocking drugs and therefore have more bound drug and produce a greater degree of conduction slowing at rapid heart rates (use dependence).ĭrugs with significant effects on potassium currents prolong the action potential duration and refractory periods. In fact, these agents largely affect potassium channels (I Kr) at normal or slow heart rates and low concentrations and therefore display “reverse use dependence” for potassium channel blockade. This means that the predominant effect on conduction (sodium channel blockade) is seen at rapid heart rates. Quinidine and disopyramide have intermediate sodium channel blocking activity and exhibit use dependence. The sodium channel blocking drugs are often called membrane-stabilizing agents because they decrease the excitability of cardiac tissue. The majority of available antiarrhythmic drugs exert predominant effects on cardiac sodium or potassium currents. Many of these drugs have effects on multiple ion channels and adrenergic receptors as well as a myriad of cardiac and noncardiovascular side effects. Given the recognition that leaving a patient in permanent AF will likely render future rhythm control therapies less effective, a strategy of sinus rhythm maintenance in younger patients is particularly worthwhile if one wishes to remain a candidate for developing rhythm control strategies.Īntiarrhythmic drugs do not lend themselves to a neat classification scheme. In addition to the aforementioned considerations, I also consider maintenance of sinus rhythm in young patients (<60 years) who have not been adequately represented in the previously cited studies and for whom the long-term implications of permanent AF are unknown. 9 This designation of rate control as the primary strategy for AF will likely be challenged with further advances in ablative and pharmacological therapies for AF. 7, 8 At present, practice guidelines recommend antiarrhythmic therapy for patients with significant symptoms despite adequate rate control. 
7 This trend has been reversed in the latter part of this decade, with an increase in rhythm control strategies driven largely by increased rates of AF ablation and an ≈2%/y increase in antiarrhythmic drug prescriptions. As a likely consequence of these landmark studies, rates of AF-associated hospitalization, cardioversion, and antiarrhythmic drug use plateaued or fell in the years after their publication. 6 Important groups of patients, including younger individuals without thromboembolic risk factors and the elderly (>80 years), were excluded from these trials, but the results were nonetheless applicable to a large percentage of the AF population. This equivalence in outcome was in part related to toxicities associated with antiarrhythmic drug therapy as well as excess stroke risk in patients in whom anticoagulation was discontinued. 1 – 5 These studies, which included primarily patients aged ≥60 years with at least 1 risk factor for stroke, failed to demonstrate a mortality benefit associated with a rhythm control strategy.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
